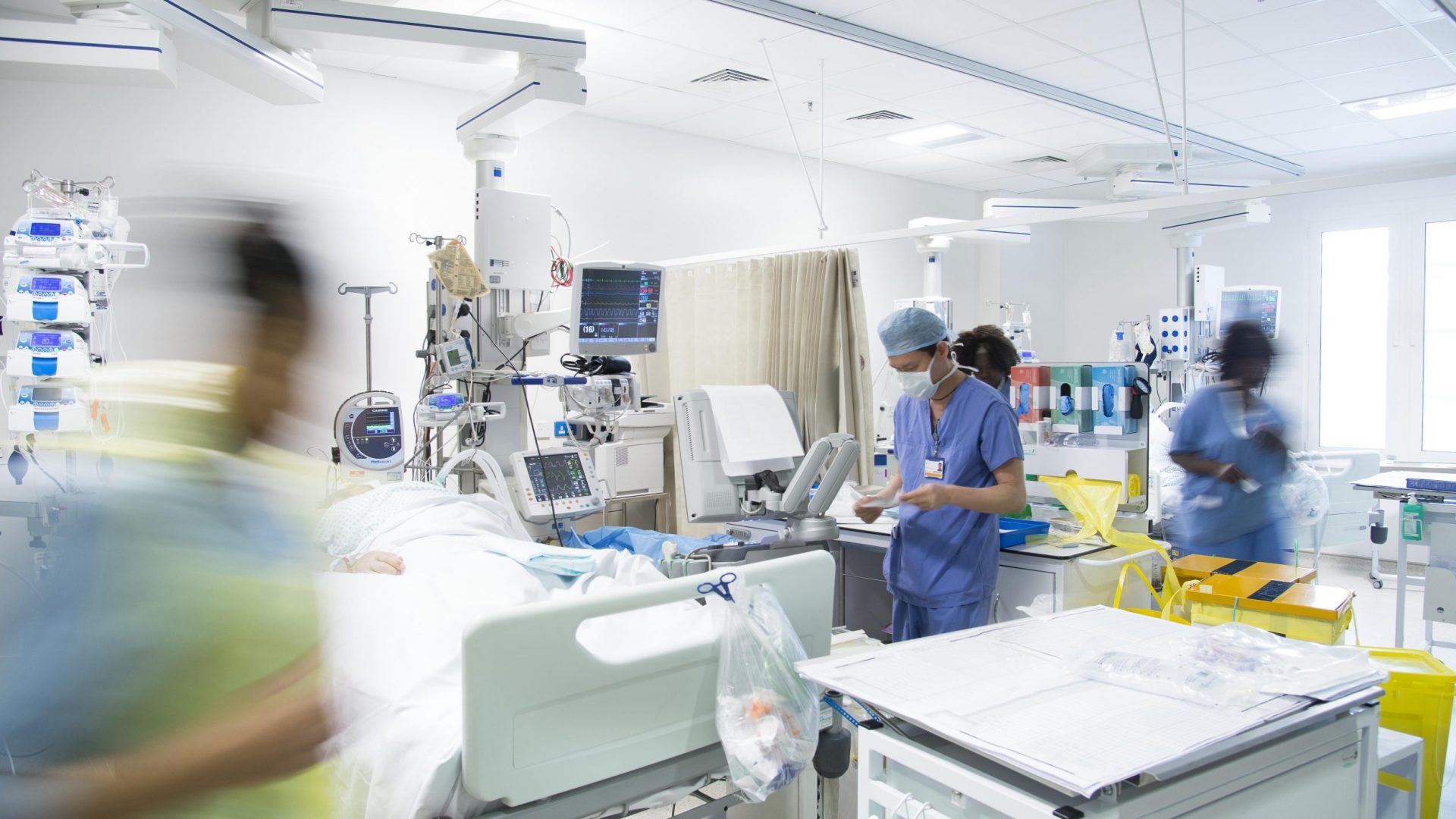
Code Red
"Since 2012, the number of people who bleed to death from their injuries within 24 hours has reduced by nearly half."Professor Karim Brohi, Professor of Trauma Sciences at Queen Mary University of London and Director of the London Trauma System
A life or death situation
These are the words of Duty Consultant, Malik Ramadhan, who coordinated the vital treatment of Niall.
Crushed by the wheels of a lorry while riding his bike, a CT scan showed Niall had blood and air leaking into his lungs that was preventing his breathing, as well as rib fractures, a broken neck and a host of other injuries.
Niall was immediately declared ‘Code Red’, a protocol introduced by The Royal London Hospital in 2008 to treat patients who have specific and severe injuries, such as major haemorrhage (bleeding) or a very low blood pressure.

Niall and the trauma team who treated him
It’s cases of life or death like Niall’s that led to the development of such trauma protocols, which are put into practice by specialist trauma teams at major trauma centres. The Royal London Hospital, where Niall was treated, is Europe’s busiest major trauma centre.
This intricate and well-established system of trauma care is what saves lives, day-in, day-out. But less than 10 years ago, this system didn’t exist.

A trauma patient recovers at The Royal London Hospital
The London Trauma System: a new approach
“Prior to 2010, trauma care in London was not organised,” says Professor Karim Brohi, trauma surgeon and Director of the Centre for Trauma Sciences.
In 2010, a novel approach was brought in: a regional trauma system – an inclusive system designed to tackle what NHS England calls “a serious public health problem”.
It’s a system that’s since proven to be highly effective. In a nutshell, the London Trauma System comprises four networks that are responsible for trauma care within their area. Each network is led by a hospital equipped with a full major trauma centre, with The Royal London Hospital – and Professor Brohi – spearheading the system.
In 2012, the same year Barts Charity helped to establish the Centre for Trauma Sciences, as part of our London’s Lifeline campaign, in London with £3 million funding, the London Trauma System model was rolled out across the rest of England. There are now 17 major trauma networks and 27 major trauma centres.

Professor Karim Brohi
A catalyst for lifesaving trauma care
Within ten years, we’ve seen the development of the Code Red protocol, the creation of the London Trauma System, and the establishment of a unique trauma research centre. The Centre for Trauma Sciences researches how we can ensure more severely injured patients survive and recover well.
Professor Brohi highlights what this has all meant for patients:
“Since 2012, the number of people who bleed to death from their injuries within 24 hours has reduced by nearly half.
“This is because we introduced the Code Red protocol, improved the type and timing of blood products given to patients, undertook earlier diagnostics and introduced damage control resuscitation surgery.
“All of these are the results of trauma research.”

Ambulance responding to a trauma incident
A growing problem
But traumatic injury – particularly major bleeding resulting from traumatic injury – is still a massive, and growing, problem. Trauma is the leading cause of death for people under 45, and a major killer of all age groups. Around 50% of patients needing a massive blood transfusion still die.
While trauma care is improving, rates of trauma also continue to increase. Researchers need to be able to tackle this increase, but public understanding of trauma – and, more importantly – how the public can help, remains low.
Mass instances of trauma, like the horrific attacks we’ve seen this year in London, and further afield in Manchester and abroad too, highlight traumatic injury on a big scale.
In the London Bridge terror attack, 36 patients were treated across three major trauma centres and two trauma units. The London Trauma System ensured the expertise and resources were available to enable effective treatment of these patients.
As Professor Brohi says, “the whole system is geared up to make order out of chaos.”
But sadly, trauma is an everyday problem. Last year, there was a 43% increase in the number of seriously injured trauma patients treated at The Royal London Hospital alone.

Trauma patient
What’s next
If one thing is clear, it’s that trauma research has the potential to unlock new knowledge of how to best treat patients. And how to do this in a way that is tailored to each patient, rather than a one-size-fits-all approach.
How can we better prevent major bleeding? What causes one patient to respond better to a treatment than another? How can we mobilise the body’s own immune system to help it fight the effects of trauma?
These are some of the questions that need answering – and some are being studied right now. The Cryostat2 trial, part-funded by Barts Charity, is uniting major trauma centres across the UK and internationally to answer whether the addition of a new drug, cryoprecipitate, early in a trauma patient’s treatment, improves their survival from major bleeding.
But there is much more to be done, and much more that can’t happen without more funding.

A researcher in an emergency room
Research in the emergency room
When Niall arrived at The Royal London Hospital in a critical state, trauma researchers were on the scene to carry out crucial tests. For them, research is not confined to the lab, but begins at the point of injury.
Emergency Medicine Doctor and PhD student, Rich Carden, speaking about the tests he carried out on Niall, said “we need to get the right blood to patients as soon as possible and give tailor-made transfusions.”
Without studying how a patient responds to different treatments from the point of injury and throughout their recovery journey, it’s impossible to drive lifesaving improvements in trauma care.
"I want to fundraise for trauma research to make sure others like me have a fighting chance."Niall, trauma patient
Why we need your help
Despite all the progress made and the new world of trauma care compared to 10 years ago, we simply have to do more. The NHS recognises the problem – we need to tackle the rise in cases of severe trauma, save more lives and improve recoveries.
Trauma research is, unfortunately, desperately underfunded. This is in part due to the limited understanding of trauma and what can be done about it.
Part of the reason why trauma is a bigger problem than ever is the modern world we live in: a world full of busy traffic (road traffic accidents), substances (alcohol can lead to falls and other accidents), terrorism (mass casualty events), violence (knife crime and other violent acts), and much.
The problem we face is why we launched our Transform Trauma appeal, supported by rapper Professor Green and it’s why we need your help. Put simply, more money means more research which means more lives saved.
Niall was one of the “lucky” ones. But for every two patients like Niall who survive major trauma, there is one who won’t.
“When I woke up I was in so much pain my family couldn’t even hug me,” says Niall. “I worried I’d never lead a normal life again.”
Fast forward several weeks and Niall is looking to the future: “I was determined to be positive; I reached milestones I never thought I’d achieve, like taking my first steps again.
“Now, I want to fundraise for trauma research to make sure others like me have a fighting chance.”
Niall is here because of trauma research. But unless we do more right now, there are far too many people who sadly won’t be.
Sources
Photo credit Sunday Mirror and Barts Charity.